
Coinsurance exampleĪfter you’ve met your deductible for the year, you have a surgery that costs $8,000. You’re responsible for the remaining 20%. An “80/20” health insurance plan means your insurance will cover 80% of the cost. In a plan’s terms, you’ll sometimes see coinsurance represented as a ratio. Since coinsurance only takes effect after you hit your deductible and, therefore, doesn’t contribute toward it. This coinsurance rate is always the same, regardless of the service or procedure. Once you’ve met your deductible, your insurance company covers a percentage of care costs, and you cover the rest. Coinsurance basicsĬoinsurance is the percentage you pay for medical costs. 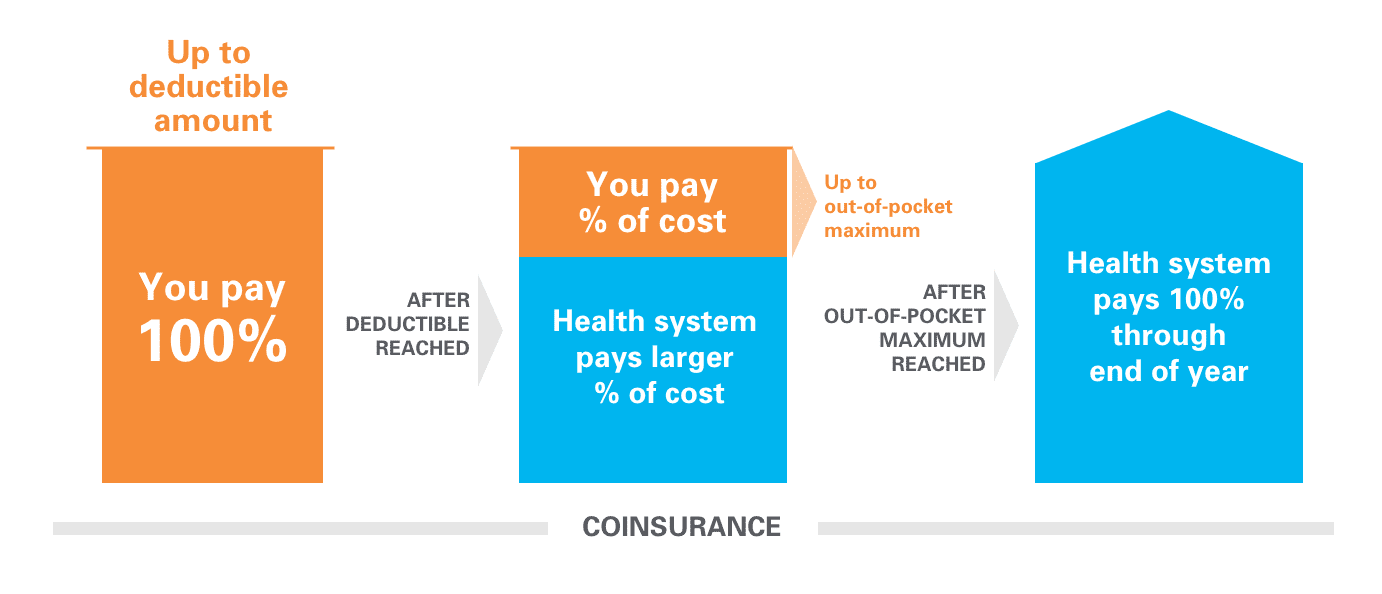
Instead of paying the entire specialist bill, you’d pay a $50 copay. Your health plan has $50 copays for in-network specialists. Say your primary care physician (PCP) sends you to a specialist to have your aching knee examined. There can also be variation among prescription drug copays, depending on the drug tier. 
An emergency room copay isn’t the same as a general provider office exam copay. It’s important to remember that there are different copays for different services. Copays usually don’t count toward your deductible. Rather than paying the entire cost, you pay the fee that your insurance company negotiated with in-network providers. This is an out-of-network provider.Ĭopayments are a fixed cost you pay for doctor visits, specialists, physical therapy, prescriptions, and any other covered medical expense. This provider is an in-network provider. When a provider doesn’t partner with your insurance company, your insurer is charged the full price for their services, raising your expenses as well. When an insurance company partners with a provider, like a doctor or a dentist, that provider agrees to a negotiated - i.e., discounted - rate for services provided to the member. In-network and out-of-network: A network is a group of healthcare providers.Insurance premium: This is the fixed amount you pay your insurance provider for coverage.When you hit your maximum, your insurance provider pays 100% of all covered services for the remainder of the year. Out-of-pocket maximum: This is the maximum amount of money you’ll pay out of pocket in a policy year.Deductible: This is the amount of money you have to pay out of pocket for covered services before your insurance begins to contribute toward the costs.To really understand how copays and coinsurance work, there are a few key terms to know: coinsurance at a glanceĪ fixed amount paid to your medical provider for servicesĬan apply before and after you reach your deductibleĪpplies only after you reach your deductible So, what’s the difference between copay and coinsurance? Let’s break it down further. Copays and coinsurance apply in different situations, but both are expenses associated with your insurance plan. Coinsurance, on the other hand, is a percentage of the cost of a service. Take the terms "copay" and "coinsurance,” for example.Ī copay is a fixed cost that an insurance policyholder pays for a specific service covered by their insurance. But understanding the terms and how they relate to one another can help you remain a savvy insurance consumer. With so many specialized terms and abbreviations, it may sometimes seem like the world of insurance has its own language.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
